
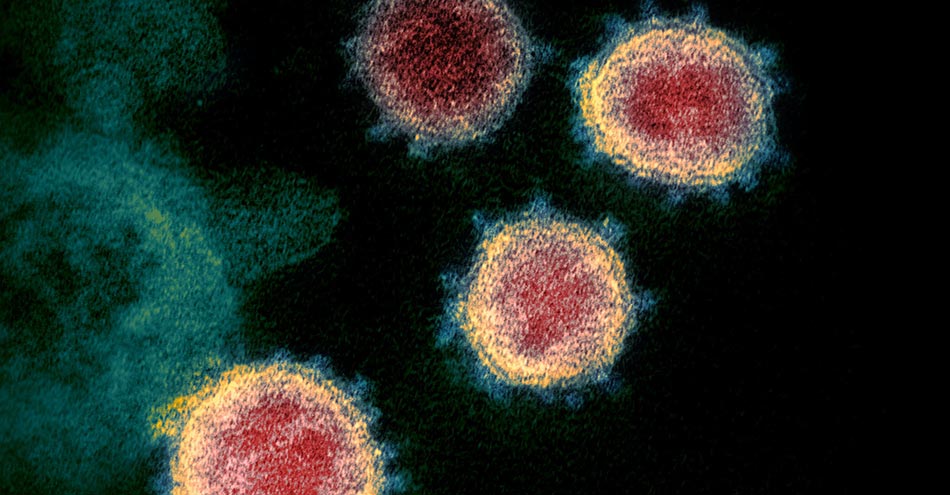
Viruses are capable of infecting the cells of other beings and cause illnesses in them. They will only show signs of life when they are in the cells of host beings and replicate. Most people consider viruses to be microorganisms. But they are not beings. Nor can they be included in the living kingdom. Therefore, virus falls in between the living and non-living world. Various types of viruses, that cause illnesses such as common cold, chicken pox, plague, polio, dengue, Ebola, and COVID-19, can be seen only through a powerful electron microscope.
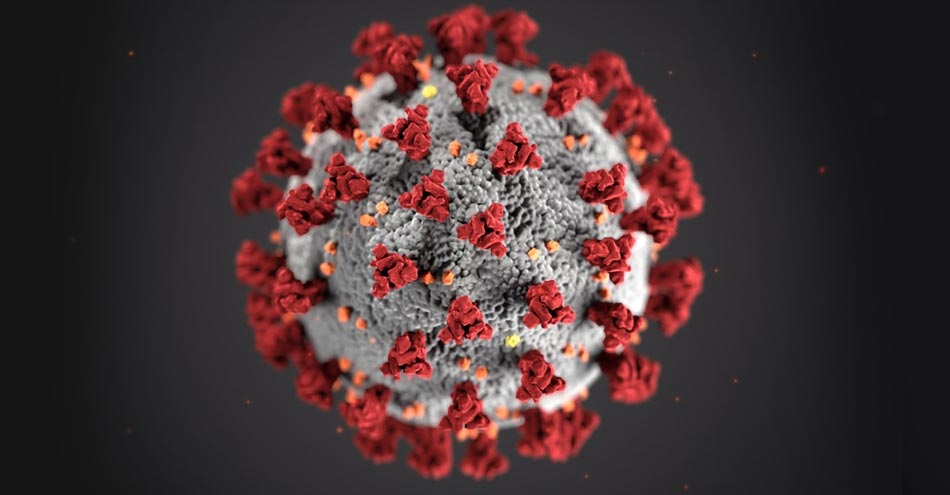
Coronavirus is a type of virus that can cause illnesses in humans from the common cold to Middle East Respiratory Syndrome (MERS), Severe Acute Respiratory Syndrome (SARS) and COVID-19. It can infect both animals and human beings. As it is covered with crown-like protein spikes, it was named Coronavirus.
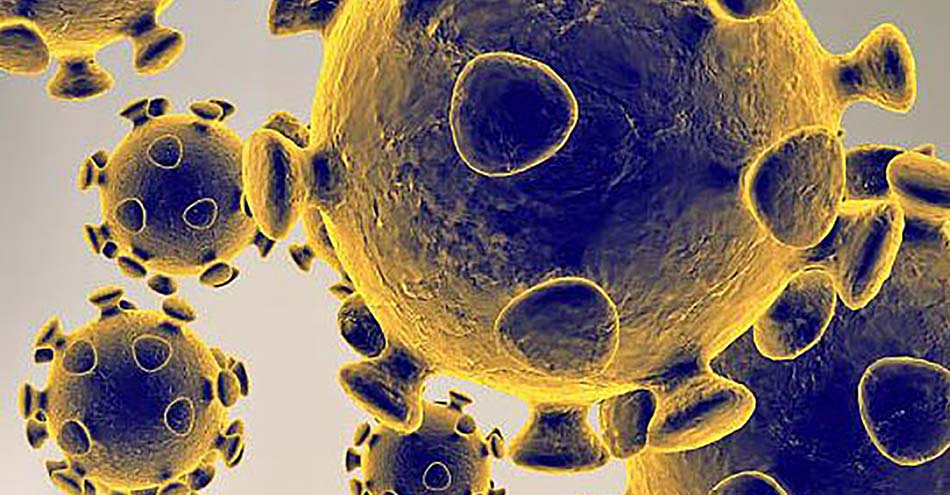
The new type of virus that was identified in China in November 2019 was named Novel Coronavirus.

Ribonucleic acid (RNA) is the genetic material of virus. This genetic material of viruses might undergo a change when they infect animals and human beings. This change that can happen over a long period of time is referred to as genetic mutation.
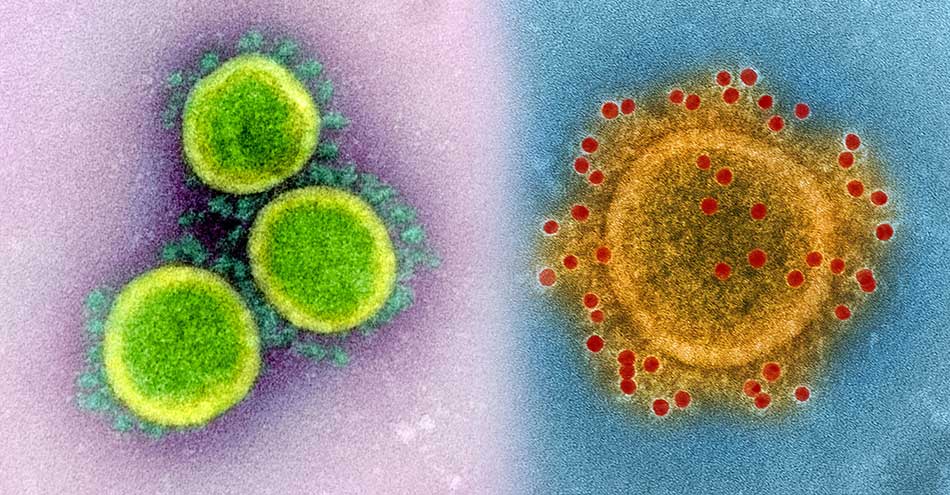
When the Coronavirus underwent a genetic mutation, Severe Acute Respiratory Syndrome Coronavirus 1 or SARS-CoV-1 was formed that caused the illness, SARS, in various parts of the world in 2003. This virus also originated in China. The MERS spread from the Middle East in 2012. The Coronavirus, inhabiting the camels, underwent genetic mutation and spread to humans, and came to be known as Middle East Respiratory Syndrome virus.
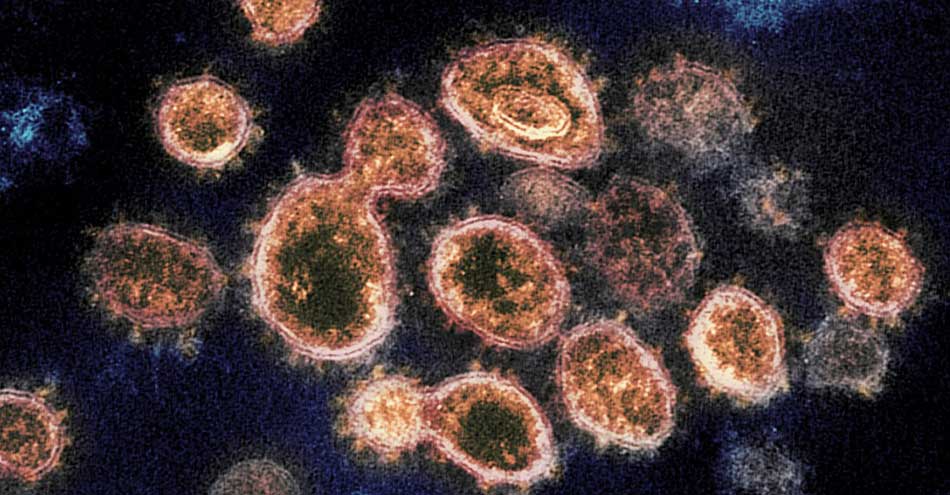
Seven types of viruses have been identified that can attack human beings. Among these, 229E (Alpha), NL63 (Alpha), OC43 (Beta), and HKU1 (Beta) can cause illnesses, including the common cold, in humans. The other three - SARS-CoV-1, MERS, and SARS-CoV-2 - undergo mutation on their own while infecting other animals and spread to humans. Severe Acute Respiratory Syndrome Coronavirus 2 or SARS-CoV-2 is the name of the virus that was identified in November 2019 in China. The SARS-CoV-2 is genetically similar to the SARS-CoV-1 that attacked China in 2002. Therefore, the International Committee on Taxonomy of Viruses (ICTV) gave it a similar name.

The disease caused by this new virus SARS-CoV-2 was named as Coronavirus Disease 2019 or COVID-19.

It refers to the disease that spreads from animals to human beings. However, there is no confirmation on which animal the SARS-CoV-2 virus passed on to humans. SARS-CoV-1 spread from bats, while MERS was transmitted from camels. The disease can spread from humans to animals too. A tiger in a zoo in New York was confirmed to have COVID-19. Anthrax, rabies, swine flu and malaria are all zoonotic diseases.

The branch of medicine that studies the diseases and health problems of a particular region by analysing the cause, patterns, distributions and determinants.

A specialised agency of the United Nations, the World Health Organization (WHO) was formed on April 7, 1948, with an objective for effective interventions in matters of health at an international level. The current chief of WHO is Tedros Adhanom. The WHO headquarters is in Geneva. China first informed the WHO about COVID-19 on December 31. The WHO declared COVID-19 as a Public Health Emergency of International Concern on January 30.

Incubation period refers to the time period from when the Coronavirus infects the body till the symptoms become apparent. The incubation period of the Novel Coronavirus is 2 to 14 days.

SARS-2-CoV-2 was first identified at the Huanan Seafood Market in the Wuhan city of the Hubei province in China. A medical student from Wuhan was the first COVID-19 case reported in India.

Patient zero is the first patient in a disease epidemic within a region or across the world. The person is also referred to as an index patient. When such a disease is first recorded, it could also be called as an index case.

Some diseases are commonly found in certain regions or specific populations. For example, common cold and fever. Though common illnesses, they rarely cause huge trouble. Such illnesses are known as endemic diseases.

An infectious disease that breaks out suddenly and spreads rapidly is referred to as epidemic. This is generally specific to a particular region. The COVID-19 became an epidemic in China only by mid-January. The Kerala government too promulgated Epidemic Diseases Ordinance in March, empowering the health department to take any stringent action in an emergency situation.

The WHO will declare a disease as pandemic when it spreads rapidly to almost all countries in the world. Most often a new virus would be spreading this illness. As humans would not have immunity against this virus, the disease would spread fast. The WHO declared COVID-19 as a pandemic on March 12, 2020, after it spread to over 100 countries.

A sudden occurrence of a disease in a particular region is called as outbreak. For example: COVID-19 broke out in China's Wuhan in December 2019. After scores of people, with a specific type of pneumonia, rushed to the hospital, the Chinese government took up the issue seriously. The disease soon spread all over China as an epidemic.

Community transmission occurs when the source of origin of a disease in a person cannot be identified and it spreads to other people. COVID-19 was reported among some people who did not make foreign trips or interact with patients. When virus infection occurs and spreads with no specific source of origin, it is identified as community transmission.

When an illness or medical condition is reported in large numbers at a specific location, it is called as a cluster. The disease would be reported among a large number of people, who reside or work in this location. This region will be called as a disease cluster. If very high number of cases are reported, it would be considered as an outbreak. If there are 10 COVID-19 patients in an area, it is considered as one cluster in India. As per this, the WHO had said in April second week that there was no community transmission in India and that only clusters were found. The cluster-level containment refers to a strategy to contain the disease spread in a specific geographical area. Strict containment measures will be taken in the area. The Union Health Ministry had said that the cluster-level containment had been effective in Pathanamthitta, Agra, Bhilwara, Mumbai, GB Nagar and East Delhi.

People with clear COVID-19 symptoms such as fever, dry cough and breathlessness are referred to as symptomatic patients. People, who have been infected but with no apparent symptoms, are referred to as asymptomatic.

The total shutdown to prevent the disease spread is called as lockdown. Those countries imposing lockdown will close all their borders. Citizens will be asked to continue at their current locations. They can only step out with special permission. Public transport will be suspended. All air-rail-water transport services will also be stopped. Only essential services and establishments will be allowed to function. The government will ease the lockdown curbs when the virus spread is contained. Nationwide lockdown was imposed in India on March 24.

Shelter-in-place directs people in a region to remain in their houses or buildings for a specific time period. This is to prevent community transmission and ensure the safety of the people. After the COVID-19 outbreak, shelter-in-place was declared for many regions in the US. Several other countries too followed suit. Shelter-in-place is also declared after bomb blasts or shootouts.

Working on official tasks at your home. IT companies mostly give this option to employees. After the COVID-19 lockdown was imposed, several companies were able to continue operations by giving the 'work from home' option to the employees. Also called as working from home (WFH).

If there are 10 COVID-19 infected people in a region, the central government considers it as a cluster. Areas with several clusters will be declared as hotspots. Regions with fewer infected people and higher death rates will also be included in the hotspot list. Pathanamthitta and Kasaragod in Kerala were on the list of hotspots released by the Centre in April first week. Rather than the number of patients, these regions were at risk of high rate of transmission. The states also have the authority to take a decision on the COVID-19 hotspots.

Depending on the COVID-19 spread, each district or regions within districts are categorised into various zones in India. As per the central government guideline, there are red, orange and green zones. A region is categorised as red zone based on the number of patients, doubling rate of cases, testing rate and surveillance data. Green zone refers to an area where not even a single case was reported in 21 days. All regions that do not fall in red or green zones will be marked as orange zone. Even in a red zone district, if no cases were reported in 21 days in the region outside the municipal limits, it would be marked as orange zone. The state governments can take a decision on changing the orange and green zone categories. But the red zones have to follow the Centre’s guidelines.

Some regions with COVID-19 patients are declared as containment zones. Mainly hotspots turn into containment zones. People will not be even allowed to step out of their homes in these zones. Police aid will be ensured for essential service. Containment zones will be declared when the virus origin remains unknown. It is mostly adopted to prevent the virus spread to other regions. Active COVID-19 cases, disease spread in the region, and possibility of further spread are factors taken into consideration by the district administration to determine these zones. If the disease spread is contained, then the curbs will be eased in the containment zones.

A person, who has returned from abroad, or has COVID-19 symptoms, will be asked to remain indoors without interacting with others. This is known as quarantine. They will not be confirmed COVID-19 patients. Also, in some cases might not show any apparent symptoms. This is a precautionary measure. Cutting of any interactions with others at home is also known as self-quarantine. In Kerala, quarantine period is for 28 days.

Those people, confirmed to have COVID-19, will be isolated from others and given accommodation at another location. Isolation wards have been set up at hospitals in Kerala for COVID-19 patents. They will have to continue to be in isolation until they recover.

When the lockdown curbs are relaxed, interactions between people will naturally increase. However, this can lead to rapid disease spread. In such a phase, the elderly people, and those with other illnesses are most vulnerable to the disease. There is also a heightened risk of the illness aggravating in such people. Those in the vulnerable category include people above the age of 60 and people with illnesses such as cancer, heart, respiratory and liver ailments, diabetes, and kidney ailments or have under undergone major surgeries. In reverse quarantine, these vulnerable people will be put under complete quarantine and healthy youths, who are less vulnerable to diseases, will be allowed to step out. The objective of the reverse quarantine is to ensure that the everyday lives of common people are not affected. It is not possible to continue lockdown in a huge country like India, especially considering the social-financial situation. In such a scenario, reverse quarantine acquires much significance.

The random testing of people in the COVID-19 hotspots and high-risk categories to check for community transmission. Even those are likely to have closely interacted with the patients and vulnerable people will be tested. Samples will be mostly collected from people such as cops on field duty, community kitchen workers, nurses, para-medical staff, delivery boys, Asha workers, people’s representatives who interacted with patients, migrant workers, and reporters. Those people turning up at the OP wing with fever and throat pain will also be examined. Sentinel surveillance helps to identify even those people, who are reluctant to share details.
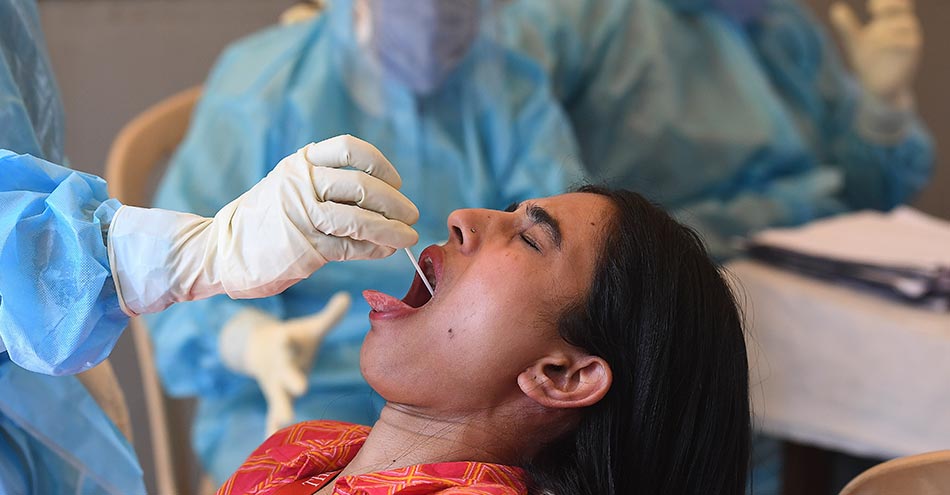
Apart from those who have returned from abroad or other states, samples are collected from the general public to identify COVID-19 cases. Cops, healthcare personnel, and those who interact with the public will be included in the augmented sample testing. The objective is to expand testing to cover more people. Authorities can take a call on who all to be included in this testing.

An individual, who can pass on the infection to several people in a large region, is called as super-spreader. The virus could spread to several other regions due to such individuals. A 70-year-old Sikh religious preacher, after returning from an European trip, had visited several villages in Punjab, spreading the disease.

Contact tracing refers to an attempt by the healthcare personnel to track down the people who had been in contact with a COVID-19 patient. The disease spread can be stopped to a large extent by finding such people and putting them in quarantine. Those with symptoms will be made to undergo tests.

The disease spreads through the respiratory droplets produced when Coronavirus-infected person coughs or sneezes (droplet transmission). These droplets can travel up to a distance of 1 metre. Therefore, if you maintain a distance of 1 metre, while interacting with others, you can prevent getting infected to some extent. Social distancing means keeping a physical distance from people at public spaces.

Special thermal screening cameras are used to check the body temperature of people. By installing these cameras at crowded places such as railway stations and airports, people with fever can be identified easily.

When a disease is declared as a notified disaster in India, then various states can use the funds from the State Disaster Response Fund to meet their expenses.

Surgical masks generally have two or three layers. These face masks are mostly available in blue or green colours. Primarily used by patients or those with symptoms. Common people, who are not at risk, can use the normal cloth masks.
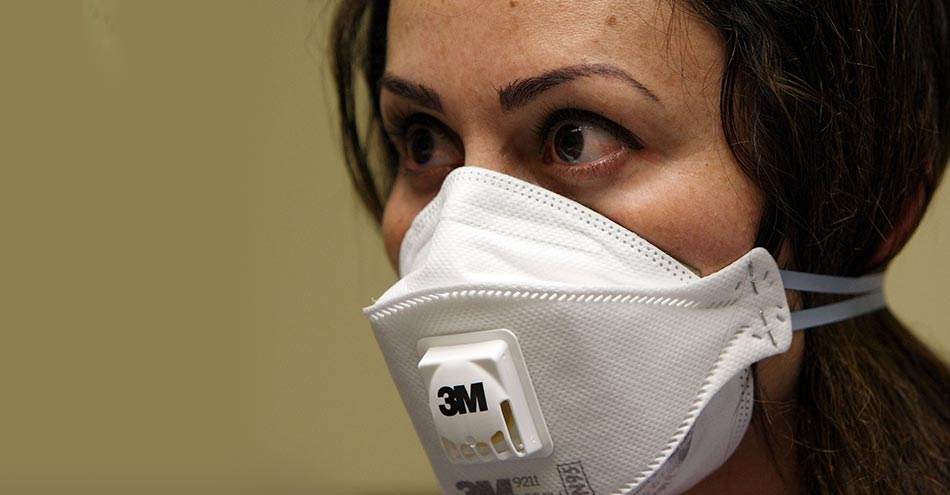
N95 Mask can filter out 95 per cent of the airborne particles. ('N' means not resistant to oil.) If used properly, these tight-fitting masks can cause some difficulty in breathing. Therefore, it is not possible to wear these for long durations. N95 masks are directed for the use of healthcare personnel or those directly in contact with the patient.
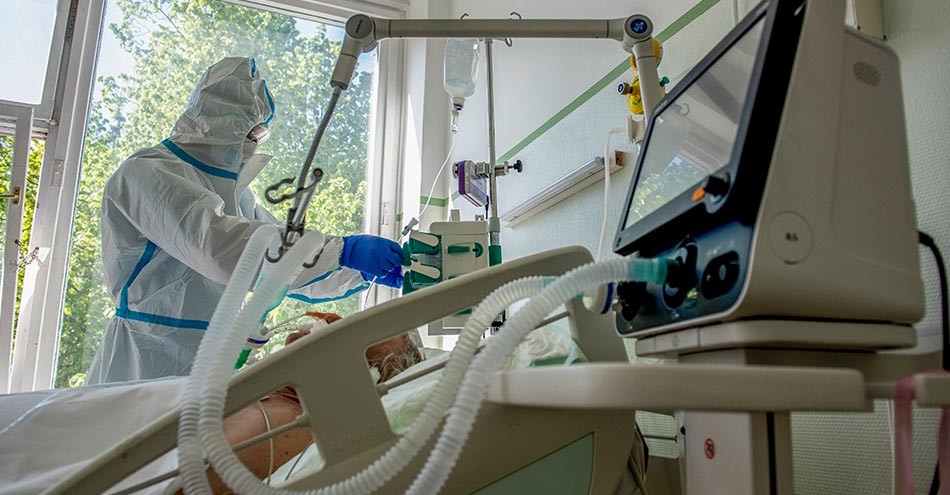
Those infected with COVID-19 will have difficulty in breathing. When they are not able to breathe on their own, they are artificially given oxygen through the life-supporting equipment, ventilator. When the patients become healthy enough to breathe on their own, the ventilator will be removed. With a spurt in COVID-19 cases, several countries faced a shortage of ventilators.
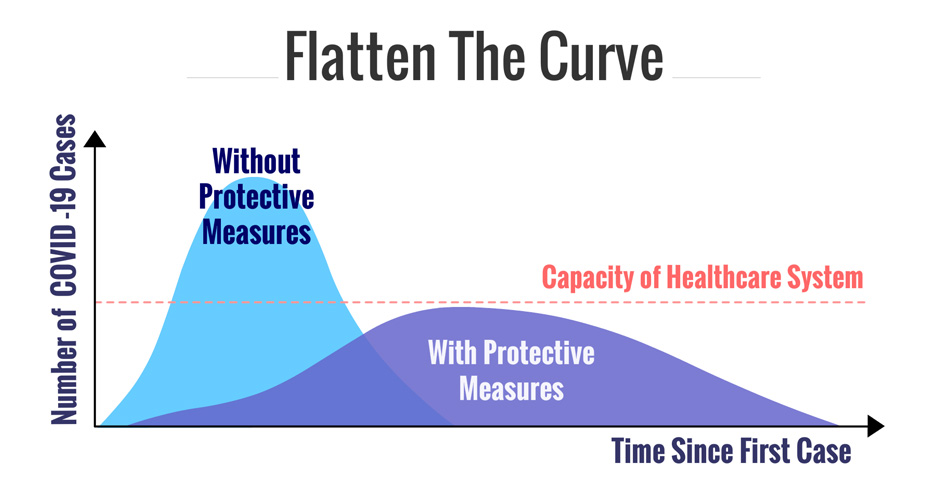
The process of containing the spread of a disease through various preventive measures is referred to as flattening the curve. These are explained using graphs. The spread of COVID-19 can be prevented by keeping your hands clean and maintaining social distancing among other preventive measures. The Center for Disease Control and Prevention (CDC) in the US put forth the framework for this. Experts in health and finance sectors depend on these charts to explain the financial situation during the epidemic days.

Indian Council of Medical Research (ICMR) is the apex body in India for the formulation, coordination and promotion of biomedical research. Funded by the central government, the ICMR is a globally renowned institution in the field of health research. The ICMR coordinates the research of various states, trying to find solutions for the challenges posed in the health sector, including COVID-
Anti-bodies can defend the body against micro-organisms such as bacteria. However, anti-bodies cannot fight virus. Vaccine helps the body to acquire an immunity against a specific infectious illness. When a disease-causing microbe, in a weakened form, enters the body through the vaccination, the immune system will be able to destroy it. The immune system will also recognise the virus if it were to infect the body in the future and fight it. There are several types of anti-virus vaccines. Inactivate virus is one among them. Virus that have been destroyed using chemicals or heat are used in this process. Polio vaccine is one example. Viruses that are grown in suitable circumstances are converted into vaccines after first weakening them. Vaccination for yellow fever is another example.
After new medicines or vaccines have been successfully experimented on animals, these are administered on human beings. This is referred as clinical trial. The experiment is done after taking the permission from each person to evaluate how effective and safe the medicine is. Only after pre-clinical testing, that includes lab tests and animal testing, has been successfully completed, permission will be given for clinical trial.

The RNA viruses such as Corona frequently undergo changes in their genetic materials. By the time, the researchers study a particular genetic structure, it would have undergone a change. The Novel Coronavirus has also undergone several genetic mutations. In such a scenario, the genome sequencing has proven to be a big challenge for researchers. A genome in a virus includes all its genes. The researchers need to identify the changes in the genome or its parts before finding a vaccine. Genome sequencing refers to the preparing of the sequence of the nucleotides in a genome, like the alphabets A, B, C, D, E... Nucleotides are the basic structural unit in an RNA or DNA.
The composition of nucleotides in each virus gene would be different. The genetic differences between them are identified by comparing these with other viruses. In such a scenario, the genome sequencing acquires significance. Genome sequencing is used to find out how the nucleotides are structured in each gene of the virus genome.

Sequencing of all the genes in the virus genome is referred to as full genome sequencing. Around 13,500 letters form this sequencing. By analysing the changes in this sequence, it can be determined if the virus has undergone mutation. The genetic mutation of the virus needs to be carefully studied. The protein cover of the virus can also undergo structural changes due to this mutation. That's how the virus protein is able to make contact with the proteins in cells of new beings. These changes in the amino acids determine how virulently can they infect others. Eight gene segments are found in the common Influenza A, B viruses. These contain the ‘instructions’ on how to attack the human body and how to produce new virus. The Coronavirus that only attacked camels underwent genetic mutation and infected humans as MERS. The virus that attacked only civets underwent mutation to become SARS-CoV-1 virus. All these became possible when the protein cover on virus underwent genetic mutation. However, the origin of SARS-CoV-2 virus has not been identified yet. By finding the genome sequencing of virus, similar virus can be found in other animals. Thus, researchers will be able to find from which animal this Novel Coronavirus spread to humans. This will also be crucial in developing a vaccine.

The medicine that made headlines after US President Donald Trump said that hydroxychloroquine can be used for COVID-19 treatment until a cure is developed. Invented in 1934, Hydroxychloroquine began to be used to treat malaria from 1947. This was found to have been effective in curing the SARS illness earlier. It is believed that the medicine can protect the human cells from the Coronavirus attack. After the demand increased, India included the medicine in the Schedule H1, making the doctor's prescription mandatory for buying it.

Personal Protective Equipment or PPE protects a healthcare personnel from an infection or any toxic substance. As per the government guidelines, the healthcare personnel in the frontline of the COVID-19 battle have to wear goggles, face shield, mask, gloves, gown, covering for head and shoe cover. All healthcare personnel in the high-risk category will have to wear the PPE.
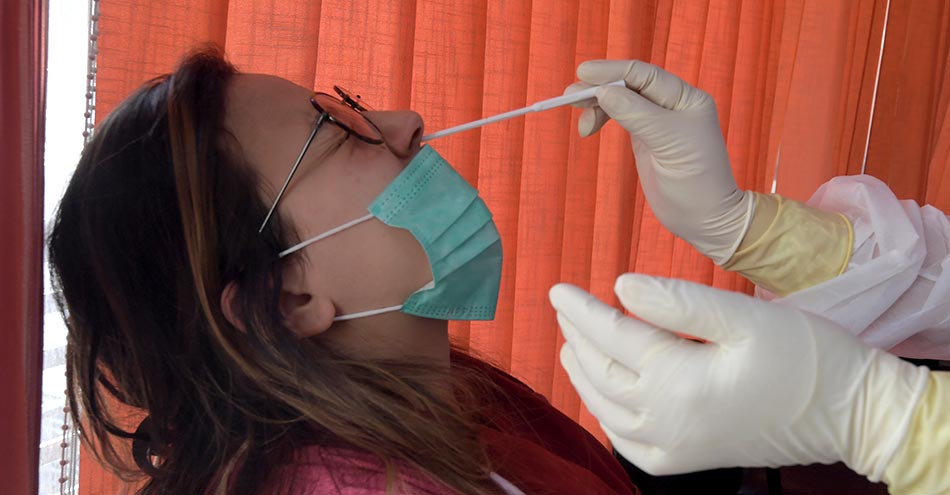
COVID-19 is confirmed in those with symptoms by testing the throat/nasal swab samples. Or sometimes the lung swabs are also taken. This will be stored in a specific temperature and taken to the lab. The reverse transcription polymerase chain reaction (RT-PCR) test is conducted to ascertain the viral infection. The samples taken from the suspected patient will include human cells, and other microbes. DNA is the basic genetic material in human cells. However, Coronavirus contains viral RNA. While the DNA is a double-stranded molecule, RNA is single-stranded. The RNA of the virus in covered by the nucleocapsid protein. The proteins help the virus to multiply in the cells. The RNA genomes give the instructions for their production. The COVID-19 tests aim to identify these genomes. N gene gives the instructions on producing the nucleocapsid proteins for the multiplication of the genomes. There should be sufficient amount of viral RNA in the sample to identify these. However, these are not usually found. Therefore, the RT-PCR amplifies the number of N genes using enzymes such as reverse transcriptase and taq DNA polymerase. The thermal cycler equipment uses the PCR method for the amplification of the DNA copy of the RNA. By analysing the information from the thermal cycler, the viral infection is confirmed. To quickly confirm the virus infection, the Real-time PCR or qPCR is used.
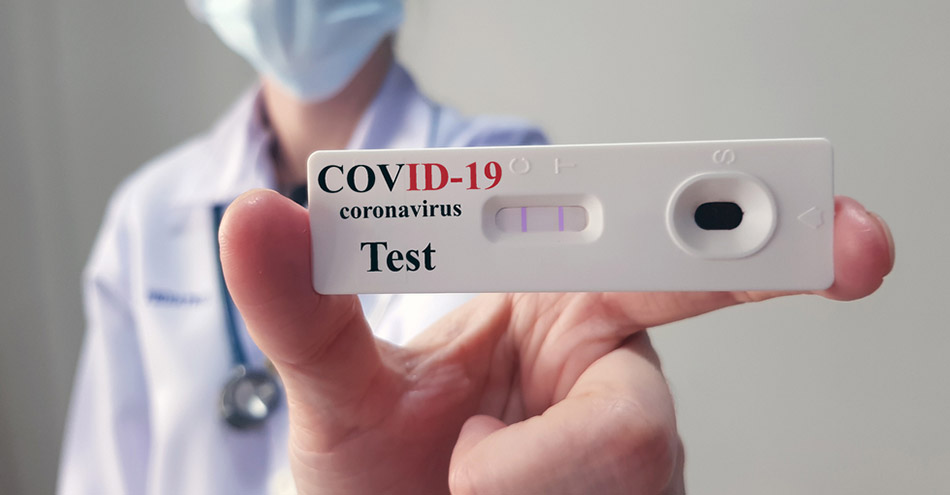
The human immunity system starts producing antibody within days of a viral infection. The rapid antibody test is to ascertain the presence of this antibody in blood. This test helps to confirm the disease rapidly, in just 30 minutes. The presence of IgM antibody confirms the illness (positive) and IgG+IGM indicates that the person has recovered (negative). However, this is just a preliminary test to identify the presence of the virus. This test is held to ascertain any type of virus infection. The rapid antibody test can only be conducted at the labs recognised by the National Accreditation Board for Testing and Calibration Laboratories. The doctor's prescription and the government nod are also needed to carry out the tests. However, only the RT-PCR tests can confirm the Coronavirus infection.

The antibody-rich plasma of a person, who has recovered from COVID-19, is used for this treatment. The plasma of the recovered person is collected and given to another patient. The antibody in this plasma will be able to fight the virus and prevent the disease from aggravating.
The most important COVID-19 preventive measure is to wash your hands using soap. Use sanitiser if soap is not available. Sanitiser with 60 per cent alcohol content is the ideal disinfectant.

The campaign started by the Kerala health department to stop the Coronavirus spread. Authorities adopted preventive measures to stop the spread of the disease from one person to another and thereby ‘breaking the chain' of the virus transmission. Ensuring hand hygiene through the use of soap and sanitiser was one of the preventive measures.

The central government's mobile application that provides health services to the Indian citizens in the wake of the COVID-19 pandemic. The app, developed by the National Informatics Centre, is used to track the COVID-19 spread, issue alert of possible threats, and create awareness. By using the GPS and bluetooth features, the app can give alert on COVID-19 regions and prevent people from interacting with infected individuals. The Centre has mandated that all government and private employees need to download the app. It is currently available in 12 languages, including Malayalam.

When infectious agents such as virus, bacteria, and fungi are artificially grown and used to spread diseases in a particular region or across the globe, they become bio-weapons. These can be used to kill others, and destroy crops, birds and animals. It has been proved that anthrax bacteria were used for such purposes. The term bio-terrorism was also formulated in this context. There are also allegations that the Novel Coronavirus was developed by China as a bio-weapon.